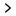It’s a difficult moment for anyone when a physician reveals that they have tested positive for diabetes type 2. It’s very normal to feel lost and devastated. Diabetes, especially Type 2, has become quite rampant for reasons like lack of exercise, genetics, obesity, and poor diet. Nowadays, it is affecting young victims as well as older ones. So medical experts and researchers are still looking into ways to eliminate both the symptoms and the condition itself.
What is Diabetes Type 2?
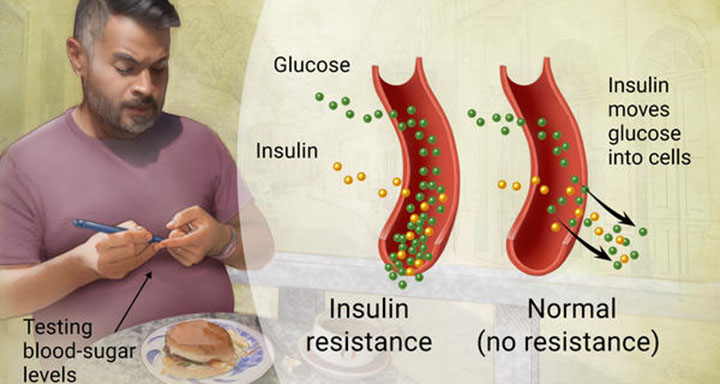
Diabetes type 2, aka non-insulin dependent diabetes, is a chronic illness that interferes with the absorption of glucose in the body. How? If you are diabetic, your body doesn’t respond correctly to insulin and fails to move glucose into cells for energy production. If the cells do not get sufficient glucose, the body’s blood levels rise and cause diabetes type 2 symptoms. Furthermore, long-term non-insulin diabetes couples with high blood glucose levels (hyperglycemia), leading to lower blood flow to the skin and causing damage to nerves and blood vessels.
Poor blood circulation leads to a reduction in collagen production which alters the skin’s appearance and its ability to heal. If your skin cells are damaged due to low collagen, you will be sensitive to temperature, pressure, and you won’t be able to sweat properly. The changes in the skin or its inability to heal quickly can be signs of a diabetes-related skin disease.

Diabetes Symptoms
There are many diabetes symptoms you should watch out for. In fact, it’s strongly recommended that you should have a formal diagnosis to confirm that your symptoms are due to diabetes. Diabetes symptoms can resemble numerous ailments. Hence, it can be a challenging task to accurately self-diagnose. Symptoms may appear gradually or all at once in some patients.
Some of the most prevalent diabetes symptoms include chronic long-term feelings of nausea and illness, candida and yeast infections, dramatic weight gain or weight loss, and abrasions that heal much slower than normal. Other symptoms are fatigue and low energy levels, frequent urination, affected vision, and an often unquenchable thirst.
Diabetes Type 2 And Skin Conditions
Diabetes is responsible for a number of fungal and bacterial skin infections. People with non-insulin related diabetes have a high risk of getting bacterial infections like boils and folliculitis. Besides that, they are prone to getting infections on their toenails and fingernails. These infections always cause inflammation and may increase in size, quantity, and frequency if blood glucose levels are consistently high. The two strains of bacteria responsible for the infections are Streptococcus and Staphylococcus.
On the other hand, diabetics also have a high likelihood of getting fungal infections like jock itch, athlete’s foot, and ringworm. These occur due to yeast or fungus and thrive well in areas that are typically itchy, red, swollen, warm, surrounded by dry scales or blisters, and sometimes with a white discharge. In addition, they also thrive well under the breasts, armpits, foreskin, and corners of the mouth.

Diabetes-Related Skin Diseases
Are you wondering what skin conditions are prevalent among type 2 diabetics? A widespread one is diabetic dermopathy, which occurs due to damage to the tiny blood vessels supplying tissues with oxygen and nutrition. Diabetic dermopathy exhibits itself with ovular or circular, light brown patches on the shins. Another common condition is digital sclerosis. Digital sclerosis causes tightening, thickening, and waxing on the skin in the joints of the patient’s hands, toes, and fingers.
Another skin condition that is specific to diabetics is disseminated Granuloma Annulare. The symptoms of Granuloma Annulare include red or skin-colored bumps and rashes on feet or hands. Acanthosis Nigricans is common among obese patients, marked by tan, brown, or gray areas of elevated skin on the groin, armpits, knees, elbows, and neck of a patient. Lastly, diabetic blisters are common among patients with nerve damage. Its symptoms include blisters that resemble burns and occur due to poor blood sugar levels.
Diabetes Type 2 Treatment Options
Several treatment options can manage the condition. For instance, insulin shots are available to those who dislike oral medication; a prescription of sulfonylureas can stimulate insulin secretion, and metformin increases insulin sensitivity while DPP-4 inhibitors regulate blood sugar levels.
If you are experiencing skin disorders due to diabetes type 2, you can opt for over-the-counter remedies like hydrocortisone, clotrimazole, and topical steroid drugs. Additionally, prescription medications to manage severe skin conditions include topical or oral antibiotics, powerful anti-fungal medicines, insulin therapy to regulate the origin of skin disorders, and more.
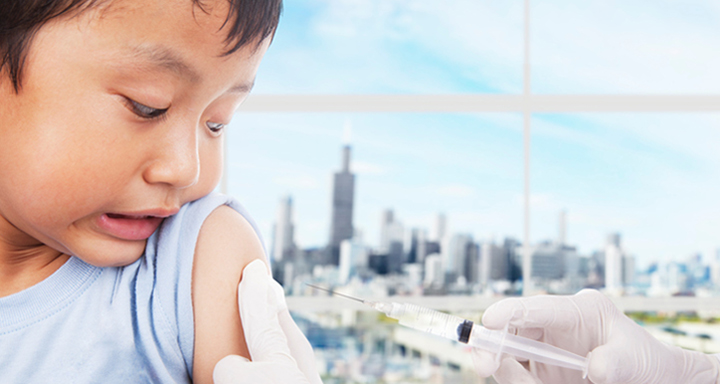
And that’s not all. Some rely on alternative remedies like talcum powder for areas of skin folds, like armpits. Also, Aloe Vera can soothe dry skin and reduce itching. Apart from these treatment options, making lifestyle changes is another way to manage the condition. Patients need to exercise frequently, stick to a diabetes diet, monitor their blood sugar, avoid scratching the dry skin, treat cuts instantly, and avoid hot showers. Before changing to a diabetes diet or changing your exercise regimen, consult with your doctor.
Outlook
Non-insulin dependent diabetes brings about numerous skin conditions. Some are harmless while others can spiral out of control if you do not seek proper and prompt management. However, if you take medications for treating the condition, embracing alternative remedies, and making lifestyle changes, you will reduce your discomfort and the severity of your condition.
A fair share of skin conditions that arise with non-insulin dependent diabetes do not cause serious harm and disappear on their own. Unfortunately, some are stubborn and can pose an enormous threat to your general health. Ensure that you make an appointment to see your doctor immediately if you have a breakout of any kind.
Featured Image Source: davidwolfe.com
Sourced from: healthline.com